“ENORMOUS RESPONSIBILITY, EVERY TIME”

The first time I saw a living brain, I was speechless: a light-grey mass, pulsing, moving in time to the heartbeat. About 1,300 grams, the center of our personality. I was a resident doctor at the time and was immediately fascinated. Today I’ve seen thousands of brains and am more experienced. But the fascination remains.
Every morning, at 6:50 am, I sit down at my desk in my office in the Solingen Clinic and use the early hours to prepare myself for the day’s scheduled operations and to plan the day with my team of three senior physicians and six residents. In Solingen, there are around a thousand operations annually in the neurosurgical department’s operating theaters, which are busy from morning until night. Of the operations, about two thirds take place on the spine—herniated discs and similar things—and one third on the brain, for instance for tumors or bleeding.
After the rounds in the intensive care unit, it starts right away. I operate daily, usually two or three operation each day. I don’t operate on the brain every day, though. I spend most of my time on the spine, which is more relaxed for both me and my patients.

When I get to the operating theater, I disinfect myself, wash my hands and collect my team for a time out. It’s like a pilot’s final check in the cockpit, during which I go through all the most important points. Meanwhile, the patient is completely covered by the surgical drapes, with just a small area of about 10 centimeters exposed. This helps me focus on my work, and the person under the sheet becomes somewhat of an abstraction. At that point I try not to think about the patient as such, but focus myself on the task that lies before me.
I take the scalpel into my hand and open the skin. Then I continue working through the microscope. Using a drill, I drill a hole into the skull and remove a piece of the bone with a finely vibrating saw. This exposes the dura mater, the dense membrane that provides additional protection to the brain. It’s not until I’ve opened this white, fibrous layer that I can see the brain. I don’t have any worries about accidentally drilling into the cerebrum: the special drill stops spinning as soon as the resistance from the skull disappears.
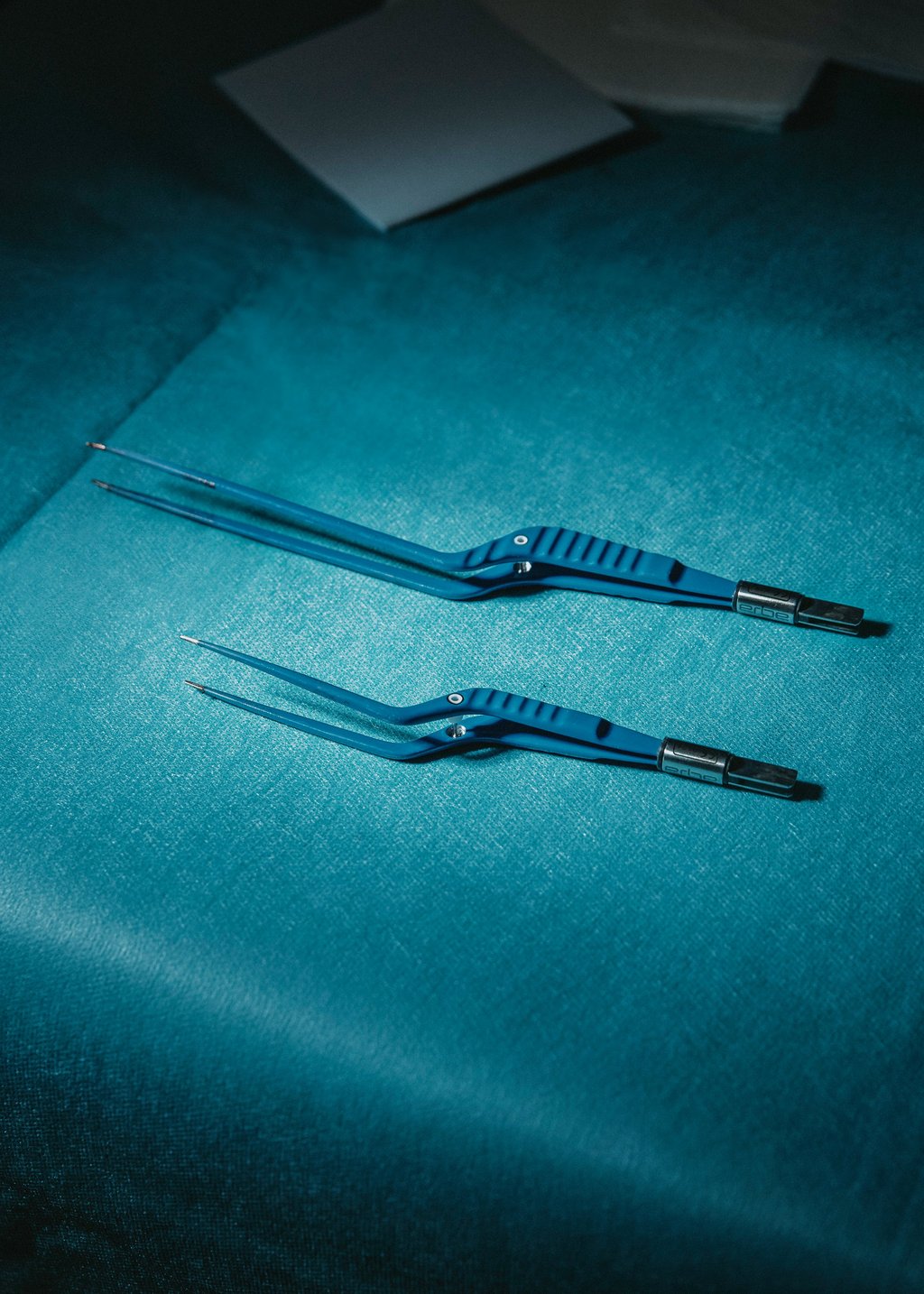
In my left hand I now hold an aspirator, to suction away the blood that immediately shoots into my field of vision. In the right hand, my strong hand—because I’m right-handed—I hold special tweezers. With the electrical current flowing through the tweezers, I can cauterize any bleeding. This way I have a clear field of vision to get to the tumor. I know exactly where it is located. The day before, I localized the culprit on three-dimensional computer tomography images and can now envision where it is located. For particularly small and more deeply located tumors, a neuro-navigation instrument helps me find them. The name of this tiny computer is Hummingbird. Thanks to its precise calculations, it can find every brain tumor, just like the eponymous bird that unerringly finds a flower’s calyx. To help it, my team feeds the computer with the previously imaged computer tomography, made up of hundreds of individual, wafer-thin, scanned electronic images.
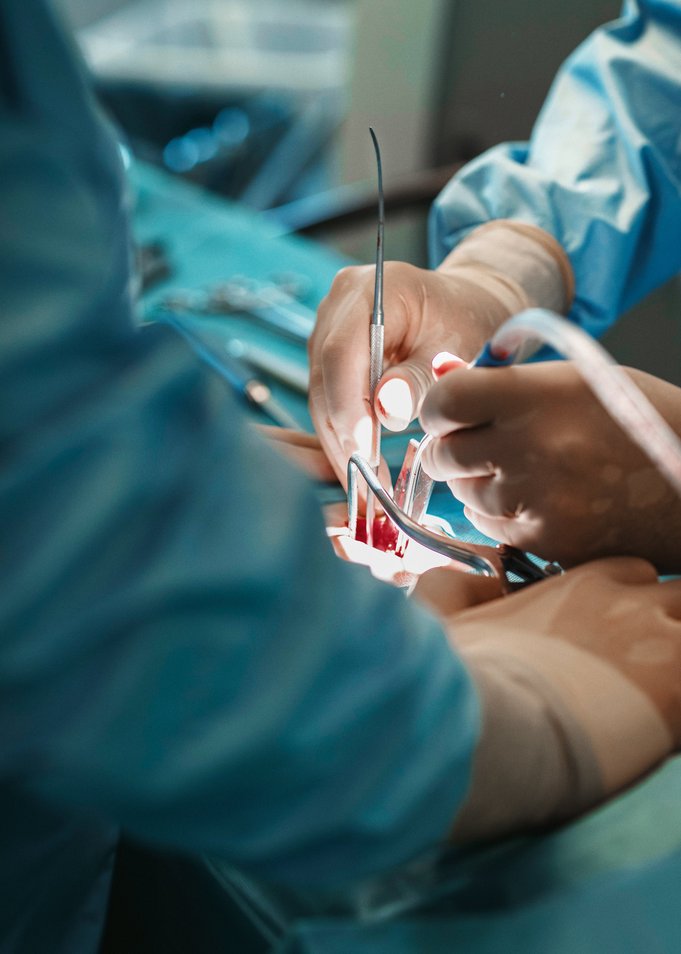
“Just a small area of about 10 centimeters is exposed.”
The patient’s head must be immovably clamped to the operating table. It’s the only way I can use laser localization to bring the brain and computer into harmony. What I then see on the screen functions a bit like a navigation system. Using an optical connection, Hummingbird shows me exactly where the tumor is located, and then I can choose the best way to access it with the least damage to healthy brain tissue.
As soon as I’ve found the tumor, I grab it piece by piece using the grasping forceps and remove it from the patient’s brain in many small steps with the help of the aspirator and the special tweezers. For especially large tumors, I work with an ultrasound aspirator, the so-called CUSA. The device shatters the tumor with high frequency sound waves, while simultaneously suctioning out the pieces and irrigating the tissue.
Both hands are now constantly in motion and yet must remain calm and meticulous. When I start a particularly complicated movement, I ask for quiet because I have to concentrate. I don’t like music in the operating theater, like some of my colleagues. I find it neither stimulating nor calming.
Once I’ve removed the tumor, I deal with stopping the bleeding. The hemorrhage cavity where the tumor was can be as large as an orange. I then fill this hole with saline solution and close the cerebral membrane. As soon as the bone is fixed back into place in the skull and the skin has been stitched closed, the operation is over and the patient can be transferred to the intensive care unit.
Complicated brain operations usually take up to four hours, while routine surgeries on the spine need two to three. After 26 years in this career, I have a lot of practice and work fairly quickly and thoroughly. My colleagues are therefore often surprised when they require two to three times as long for similar operations. But thanks to decades of experience, the hand movements are automatic and certain. And especially for emergencies, which happen time and again, this speed counts. For strokes and arterial aneurysms, the operation must occur within sixty minutes and the bleeding stopped, otherwise the patient will die or there will be serious complications. These emergency operations on the brain are unpredictable and extremely difficult.
But even the normal operations on the spine aren’t without their risks. If I make a mistake, the patient can end up in a wheelchair. It’s an enormous amount of responsibility that I feel with every single operation, whether it’s on the brain or the spine, whether I have a child or an older person lying on the operating table.
The patients come to me and place their fate in my hands. They place their trust in me. And I must therefore also have trust in myself and in my abilities. I have to know myself and my reactions extremely well.
Despite this, I don’t consider myself a control freak. I don’t have to compulsively plan everything down to the tiniest detail. My strengths are my inner peace and the calmness that comes over me before a surgery. I find that perfectionism or too much control tends to limit you. I build on my peace and my experience and have done very well with this so far. It allows me to gain the necessary distance—and to clear my mind.
“As clichéd as it sounds, practice really does make perfect.”
I’m often asked if I am afraid of making a mistake. In fact, I’m not afraid, otherwise I wouldn’t be able to do my job responsibly. In my opinion, the best remedy against fear is experience. The more often you’ve performed an operation, the more secure you become. As clichéd as it sounds, practice really does make perfect.
Nevertheless, I still have respect for complicated operations. If I know a complex operation is imminent, I give it a lot of thought in advance. And then I naturally also feel a certain amount of tension.
When something goes wrong during an operation or a patient dies, I’m very affected by it. This is fortunately a rare occurrence, but then I carry these cases around with me for some time. Then I find myself classically reimagining the procedure and thinking about what I could have done differently to save the patient. It’s difficult to accept that you always give your best as a surgeon and sometimes it still isn’t enough. That just a few millimeters too many can lead to an unexpected hemorrhage. But unfortunately this danger is always part of it.
If I can draw something positive from this, then it’s that I’m that much more thankful for my health and the health of my family. Because being healthy isn’t something I just take for granted. Once I even operated on my own father. That’s really something that you shouldn’t do. He had a spinal canal constriction and problems walking. Of course he could have had the surgery somewhere else, but I wanted to do it myself. Then when my father was on the table in front of me, I was twice as tense. I knew that my own father was lying beneath the sheets. But my father had trust in me. And I trusted that I could do it. It all worked out fine.
Even after 26 years as a surgeon, I learn something new every day and experience unusual moments. Operations on patients who are awake, for instance. When the tumor is located in an important region, for instance in the language or movement center, then by using electrical impulses during the operation you can determine where you have to be especially careful. The patients are shown pictures during the operation that they have to identify. Or they play an instrument. As soon as their speech or movement becomes impaired, I know that I have to stay away from that area.
Many people don’t know that our brains can’t feel any pain at all. That means that I can talk to the patients without any problems. Just the protective membrane needs to be lightly anesthetized, but you can cut into the brain itself without the patient noticing.
There was one operation in my career that I will never forget. It lasted seven hours. There was a woman on the operating table with a benign tumor right between the cerebellum and the spinal cord, at the junction between the brain and the cervical spine. And there’s just not a lot of space there. I had to take a lot of extra time, work extremely slowly and carefully, stay focused. One mistake and the woman would have lost her freedom of movement. But luckily everything went well.
To this day, that patient visits me and gives me a present every year around Easter. Such small gestures show me how wonderful it is to live up to your responsibility and to uphold the trust that others have placed in you."